What is Radiofrequency (RF) Neurotomy?
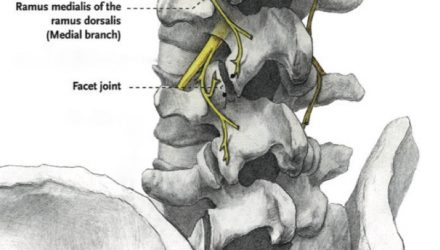
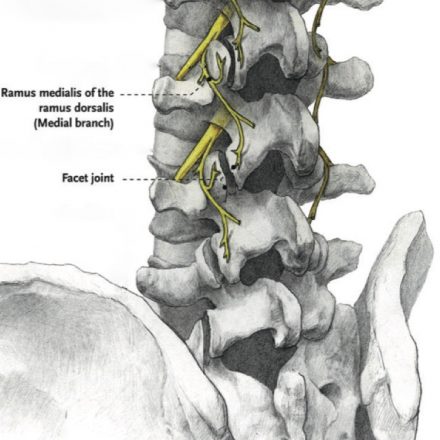
Radiofrequency neurotomy or ablation is a procedure that is performed to reduce transmission of pain through very small nerve branches that supply the spinal facet (or zygapophysial) joints as well as the sacroiliac joints.
These joints are bilateral and are subject to painful osteoarthritis, particularly in the neck and low back where they are weight-bearing joints. Degeneration of these joints is a common cause of low back and neck pain.
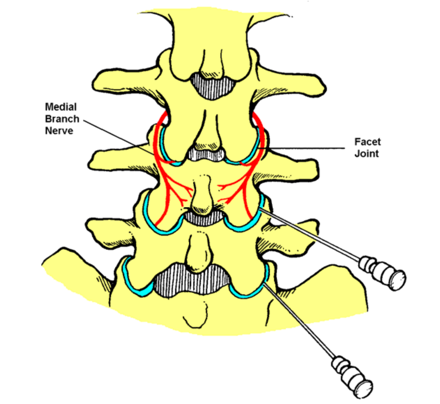
Radiofrequency neurotomy involves applying a high-intensity electric field from the tip of a specialised, insulated needle placed as close as possible to the target nerve. This heats the tissues around the tip of the needle causing a heat lesion of the nerve branch, although the electric field has other direct effects on the nerves. Each joint is supplied by more than one nerve, hence multiple lesions are usually performed together.
How is the procedure performed?
The procedure is performed in an operating theatre as a day-only stay.
Performing the procedure itself requires about half an hour but you will need to arrive about an hour before the procedure to be prepared for theatre.
A specialist anaesthetist will care for you throughout your procedure. Your anaesthetist will place an intravenous cannula (“drip”) in your hand or arm and administer sedation and oxygen appropriate to the procedure whilst monitoring your vital signs.
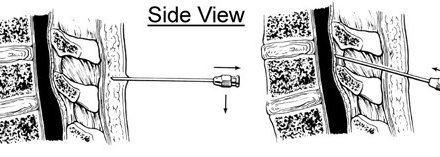
You will be asked to lie face down. Padding will support your head, arms, chest and legs. The procedure will be performed using a sterile technique which involves use of antiseptic solution on your skin, sterile drapes and gloves. X-rays and nerve stimulation will be used to place the needle as close as possible to the target nerve. Nerve stimulation also serves to protect you from damage to other structures. The skin will be numbed with local anaesthetic before the special needles are inserted. Long-acting local anaesthetic will be injected through the needle at the end of the procedure.
(Diagram acknowledgement: Faculty of Pain Medicine, ANZCA)
What is the likely outcome?
Radiofrequency neurotomy may reduce pain for many months.
The average is 6 – 12 months but sometimes it lasts longer. This period of reduced pain is often useful to facilitate other therapies (such as active physical therapy or increasing an exercise programme) or to reduce use of harmful medication. However, the nerve eventually recovers from the procedure and the pain may return. If helpful, the procedure can be repeated, often with similar results.
What are the potential complications?
The procedure is very safe but there are always risks of adverse effects.
Common, short-lived adverse effects include:
- pain and bruising at the site of the needle insertion.
- temporary numbness and weakness from local anaesthetic.
Uncommon adverse effects include:
- bleeding from the site of the needle insertion.
- infection at the site of the needle insertion.
- nerve irritation resulting in a temporary burning sensation (up to 6 weeks).
Rare adverse effects include:
- nerve damage with lasting effects such as numbness, pain or weakness.
- damage to other structures, depending on site of treatment
- punctured lung for intercostal nerve procedures.
- severe reactions to medications.
- complications related to sedation (please discuss this with your anaesthetist).
How do I prepare for the procedure?
At the time of booking your procedure it is important that you declare if you:
- are taking any blood thinners, including over-the-counter medications.
- are taking medication for diabetes, especially insulin.
- have an implanted device such as a pacemaker or stimulator.
- could be pregnant (x-rays and medications may cause harm).
A few days before your procedure it is important that you:
- organise an adult to accompany you from hospital and stay overnight with you.
- notify your anaesthetist if you are unwell.
On the day of your procedure it is important that you:
- have nothing to eat for at least 6 hours before your admission time.
- may drink small amounts of water up until 2 hours before your admission.
- take your usual medications unless otherwise instructed.
- have a shower on the morning of the procedure.
What happens after the procedure?
You will recover from your sedation under specialised nursing care. Local anaesthetic from the procedure should minimise post-procedural pain. When it is safe, you will be discharged into the care of an adult. For the next 24 hours you should not drive or operate machinery, care for young children alone or conduct important business.
As the local anaesthetic wears off, your post-procedural pain may increase for a few days and may persist for a week or so. Most people can differentiate post-procedural pain from their chronic pain.
If you have any unexpected symptoms or side effects following the procedure you should contact your Brisbane Pain Medicine specialist, your family doctor or your nearest emergency department immediately.